CU Stays on Track to Support Rural Health Care Needs
School of Medicine program offers hands-one learning in small communities

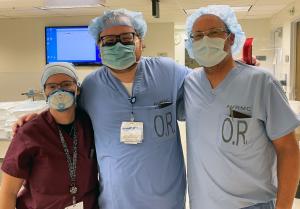
SOM Rural Track students at Mt. SanRafael Hospital
Despite population growth in the tens of thousands over the past few years, two-thirds of Colorado’s 64 counties remain rural or frontier. Frontier counties have fewer than six people per square mile. The problem is, nearly all of those counties are short on access to primary care, dental care and mental health services.
For 17 years, the University of Colorado School of Medicine Rural Program has been a pivotal part of the solution. The program was founded to attract, admit and support students who aspire to practicing in rural communities after they finish their training. A key feature of the program is a partnership with rural communities across the state in which Rural Program students obtain a significant amount of their clinical training. The host rural communities have the opportunity to recruit the Program’s students to their future medical staffs. CU is a recognized national leader in rural medical education; only about one-fourth of U.S. medical schools have similar programs.

Dr. Mark Deutchman
According to the Health Professions Services Administration, there should be at least one primary care provider for 3,000 or 3,500 people. By that standard, Colorado would need 260 additional primary care providers, Deutchman said.
“However, that number is widely disputed as being inadequate to provide all the preventive care and illness care that a population should be able to access,” Deutchman said. “A ratio of 1,500 people to one primary care physician is more accurate in the modern health care system. That would double Colorado’s estimated shortage to over 500.” Because of this ongoing shortage, the School of Medicine’s Rural Program has been applauded for making an important contribution to health care in rural communities.
The Rural Program has a part-time staff of four physicians, a manager and three coordinators to serve the 80 students enrolled in the program during any given year with about 20 students in each of the four years of medical school.
Deutchman explained the Longitudinal Integrated Clerkship, or LIC, is the core clinical year that students spend in a rural community.
“LIC is part of the new School of Medicine curriculum for all students, but our students are the only ones who complete that in rural sites,” he said.
Mandy Swanson, MD, one of those physicians serves both as a rural preceptor for students and as longitudinal integrated clerkship (LIC) liaison for the Eastern Plains. She says that as LIC students support the clinic and the community, she delights in seeing them develop over a longer period of time.
Dr. Mandy Swanson, left, with Rural Program student Michael Persinger and another colleague in LaJunta, Colorado.
It also adds to the family environment of addressing the needs of residents in rural areas.
“Having a student on a daily basis mostly adds a lot of fun to our clinic. It allows me to have the students do a deep dive into a complicated patient that I don’t have the time for,” Swanson said. “I call it my anti-burnout medicine. They help me see the fun and the excitement and the newness of medicine that sometimes it is easy to forget after you have been in practice for a while.”
The rural program actively prioritizes recruiting students from smaller Colorado communities so they may return to their own communities or other frontier areas, Deutchman said. That’s part of what appealed to Gabrielle Coleman, a second-year medical student from Parachute, Colorado.
“My dad is a family medicine physician, so I grew up watching him be the small-town doctor. Pretty much everybody in town knew him and would talk to him at the grocery store and show him their rash or whatever . . . and, he loved it,” Coleman said. “That always meant a lot to me, and I just really enjoyed watching him doing that growing up.”
Coleman planned on following in her father’s footsteps from an early age.
“The fact that CU has this program and it’s really based on mentorship and teaching students about what it means to live and work in a rural community – the special considerations – it seemed like the perfect fit for me,” he said.
Coleman is doing her LIC in Fruita, Colorado, only an hour from her home in Parachute, and will be living there with her grandparents.
“I also love the hospital system over there,” she said. “I was born in Grand Junction. So, I get to do OB in the town I was born in for the first time, which is pretty cool.”
Having family in rural areas has also piqued the interest of students such as Dakota Hitchcock, a second-year medical student from Littleton, whose mother’s family is from Alamosa, Colorado.
“I knew early on that I wanted to work with underserved populations, and rural seemed like an opportunity to do that,” she said. Her LIC placement is in Alamosa where she is excited to be staying with her grandmother.
“I am also really excited to become part of a small community and really get involved with the community,” she said. “I think that it’s hard when you are in a city to get involved with a good amount of people and I think this opportunity will allow me to do that.”
Rural and Frontier communities have much to be excited about in addition to the influx of CU rural program students. With the 2022 passing of Senate Bill 22-172, the Colorado Rural Healthcare Workforce Initiative, the state as a whole has acknowledged the dire need to increase the number of health care professionals practicing in Colorado's rural areas and is taking steps to fix the discrepancy. Deutchman wrote and directed the initiative which is designed to include nursing, dentistry, public health and behavioral health.
“It extends the best practices of our rural program to other health professions across Colorado,” Deutchman said. “As far as I know, Colorado is the first state to try to do this.”
Deutchman and other advocates for rural health, including those who helped pass Senate Bill 22-172, are looking to create balance in health care across Colorado.
“There are also regional disparities exacerbated by the fact that physicians and other health care professionals are relatively over-supplied in cities and relatively under-supplied in rural areas,” he said. “This reinforces the importance of programs like ours that attract, admit and nurture students who actually want to go to work in rural areas.”
Graduates of CU’s rural track are currently practicing medicine across the state in communities like Cortez, Pagosa Springs, Gunnison, Salida, Sterling, Del Norte and Walsenburg.
“Our overarching goals are to help our students understand what rural life and rural professional work is really like,” Deutchman said. “We provide them with a broad and deep knowledge of rural life and practical experience and teach them about the structure of rural communities, rural health care issues, skills and attitudes that will be helpful in prospering in rural practice – and also in their personal and professional identity formation.”
Learn more: https://medschool.cuanschutz.edu/ruralprogram




